Dr. Vishaj S. Maru
Dental Practitioner
Mumbai
Diabetes is a metabolic disease that causes high blood sugar. The hormone insulin moves sugar from the blood into the cells to be stored or used for energy. With diabetes, body either doesn’t make enough insulin or cannot effectively use the insulin. Whether you have type 1 diabetes or type 2 diabetes, managing your blood sugar level is key.
The higher blood sugar level, the higher is the risk.
When you have diabetes, high blood sugar can take a toll on your entire body including teeth and gums. The most common oral health problems affecting people with diabetes are:
With increased blood glucose levels, individual may have more glucose in their saliva and very dry mouths. These conditions allow dental plaque to build up on teeth, which leads to TOOTH DECAY AND CAVITIES.
Diabetes reduces your ability to fight bacteria. If plaque is not removed with regular brushing and flossing, it’ll harden under the gum line into a substance called tartar (dental calculus). The longer plaque and tartar remain on the teeth, the more they irritate the gums. Gums become swollen and bleed easily. Which is called GINGIVITIS.
PERIODONTITIS tends to be more severe among people who have diabetes because diabetes lowers the ability to resist infection and slows healing. An infection such as periodontitis may also cause your blood sugar level to rise, which in turn makes your diabetes more difficult to control. Preventing and treating periodontitis with regular dental cleanings can help improve blood sugar control. Thus gingivitis can lead to a more serious infection called periodontitis, which destroys the bone and soft tissues that support your teeth. Eventually, periodontitis cause your teeth to loosen and possibly fall out.
People with diabetes may be more likely to develop ORAL THRUSH, which is a fungal infection caused by the yeast Candida Albicans. Signs of thrush include painful white or red patches inside your mouth. Maintaining a good oral hygiene can help you avoid thrush.
TASTE DISTURBANCES is a critical component of oral health that is affected adversely in patients with diabetes. This sensory dysfunction can inhibit the ability to maintain a proper diet and can lead to poor glycaemic regulation.
People with diabetes complain of XEROSTOMIA (dry mouth). Xerostomia complaints may be due to thirst, a common manifestation of diabetes.
To help prevent damage to your teeth and gums, take Diabetes and Dental Care seriously:
- Make a commitment to manage your diabetes.Monitor your blood sugar level, and follow your doctor’s instructions regularly. The better you control your blood sugars, the less likely you are to develop gingivitis and other dental problems.
- Brush your teeth at least twice a day.
- Use a soft-bristled toothbrush and toothpaste that contains fluoride.
- Avoid vigorous or harsh scrubbing, which can irritate your gums.
- Get a new toothbrush at least every three months.
- Floss your teeth at least once a day.Flossing helps remove plaque between your teeth and under your gum line.
- Schedule regular dental visits.
- Make sure your dentist knows you have diabetes. Make sure your dentist has contact information for your doctor who helps you manage your diabetes.
- Look for early signs of gum disease.Report any signs of gum disease including redness, swelling and bleeding gums to your dentist. Also mention any other signs and symptoms, such as dry mouth, loose teeth or mouth pain.
- Smoking increases the risk of serious diabetes complications, including gum disease and ultimately, loss of your teeth. If you smoke, ask your doctor about options to help you quit.
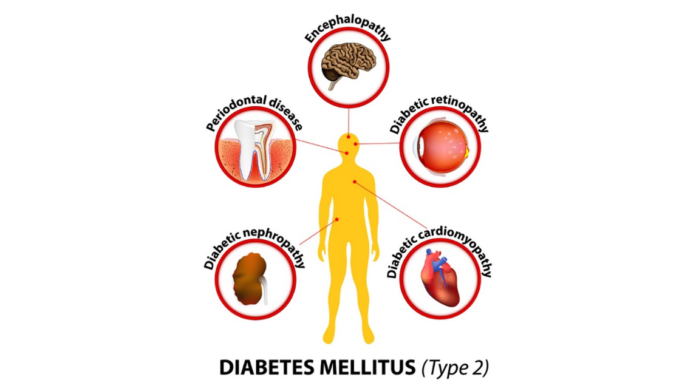
Diabetes mellitus affects people of all ages, and its prevalence has been increasing. Providing safe and effective oral medical care for patients with diabetes requires an understanding of the disease and familiarity with its oral manifestations.